|
Back to Blog
Phoenix viewer eye movement6/2/2023 
Pseudotumor cerebri: brief review of clinical syndrome and imaging findings. Diagnosis and management of cerebral venous thrombosis: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Saposnik G, Barinagarrementeria F, Brown RD Jr, et al. Imaging diagnosis of dural and direct cavernous carotid fistulae. 
Dos Santos D, Monsignore LM, Nakiri GS, Cruz AA, Colli BO, Abud DG. Diagnosis and treatment of dural carotid-cavernous fistulas: a consecutive series of 27 patients. Théaudin M, Saint-Maurice JP, Chapot R, et al. Dural carotid-cavernous fistulas: epidemiology, clinical presentation, and management. IgG4-related disease of the head and neck: CT and MR imaging manifestations. Fujita A, Sakai O, Chapman MN, Sugimoto H. Radiographic patterns of orbital involvement in IgG4-related disease. Correlation of MR imaging findings and clinical manifestations in neurosarcoidosis. Neurosarcoidosis: review of imaging findings. Lury KM, Smith JK, Matheus MG, Castillo M. Tolosa-Hunt syndrome: MR imaging features in 15 patients with 20 episodes of painful ophthalmoplegia. Schuknecht B, Sturm V, Huisman TA, Landau K. MRI findings in Möbius syndrome: correlation with clinical features. Congenital innervation dysgenesis syndrome (CID)/congenital cranial dysinnervation disorders (CCDDs). Magnetic resonance imaging features of two cases of acquired Brown’s syndrome. Siegel LM, DeSalles NL, Rosenbaum AL, Demer JL. Computed tomography in the evaluation of Brown syndrome of the superior oblique tendon sheath. Mafee MF, Folk ER, Langer BG, Miller MT, Lagouros P, Mittleman D. MRI in congenital Brown’s syndrome: report of 16 cases. Brown’s syndrome: diagnosis and management. Fourth cranial nerve palsy and Brown syndrome: two interrelated congenital cranial dysinnervation disorders? Curr Neurol Neurosci Rep 2013 13(6):352. MRI findings in Duane’s ocular retraction syndrome. Xia S, Li RL, Li YP, Qian XH, Chong V, Qi J. Congenital cranial dysinnervation disorders: a concept in evolution. 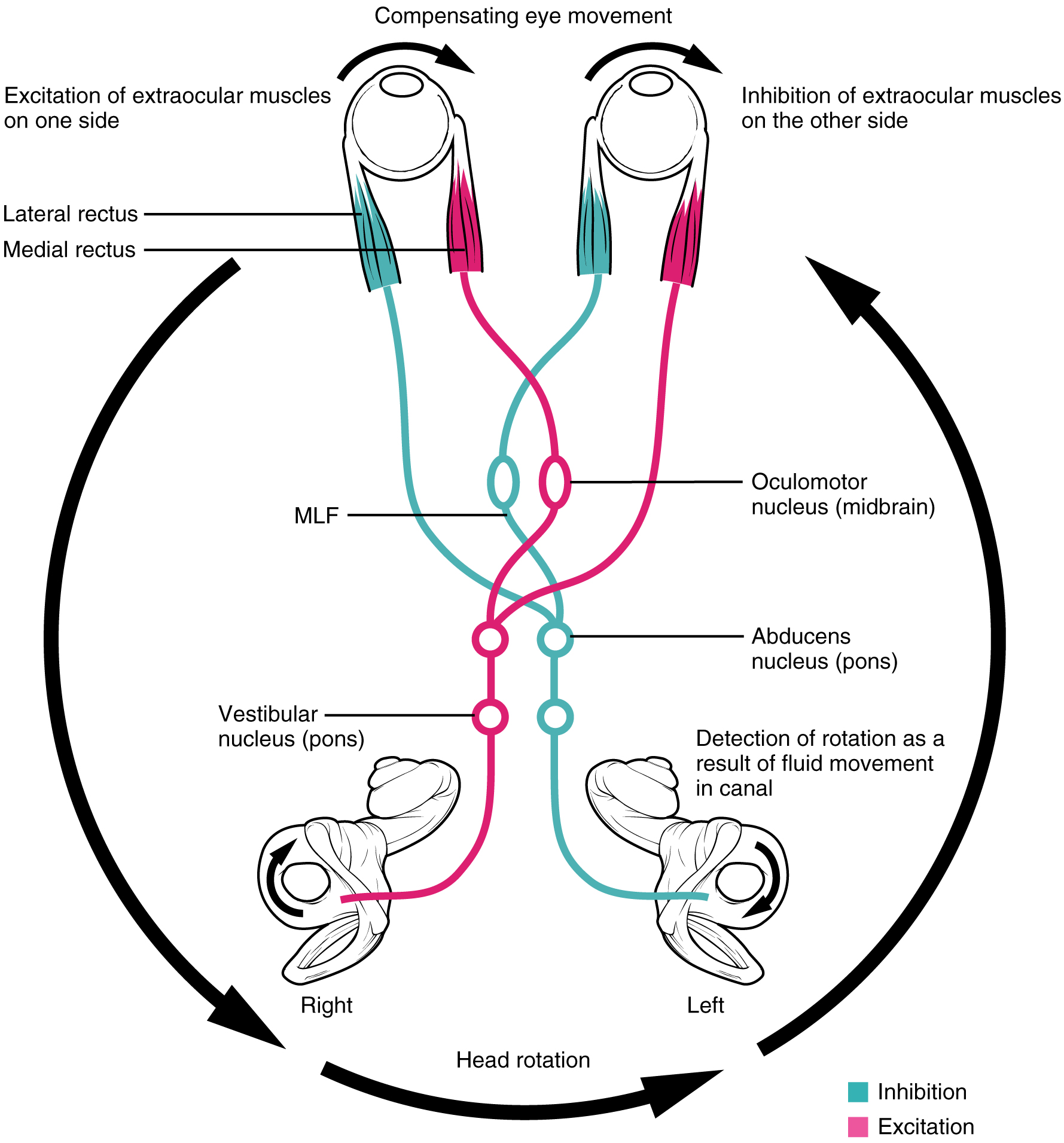
Surgical treatment of supranuclear and internuclear ocular motility disorders. Botulinum toxin in the management of internuclear ophthalmoplegia. Murthy R, Dawson E, Khan S, Adams GG, Lee J. Wall-eyed monocular internuclear ophthalmoplegia (WEMINO) with contraversive ocular tilt reaction. 
Jeon SB, Chung SJ, Ahn H, Lee JH, Jung JM, Lee MC. One-and-a-half syndrome in pontine infarcts: MRI correlates. de Seze J, Lucas C, Leclerc X, Sahli A, Vermersch P, Leys D. A neuro-ophthalmological analysis in 80 cases of multiple sclerosis. Tsuda H, Ishikawa H, Matsunaga H, Mizutani T. Neuro-ophthalmology: diagnosis and management. Eye movement disorders: third, fourth and sixth nerve palsies and other causes of diplopia and ocular misalignment. In: Netter’s correlative imaging: neuroanatomy. A thorough understanding of central nervous system anatomy, cranial nerve pathways, and orbital anatomy, as well as familiarity with patterns of eye movement restriction, are necessary for accurate detection of radiologic abnormalities that support a diagnostic source of the suspected extraocular movement disorder. Specific causes of ocular dysmotility can be localized to the cranial nerve nuclei in the brainstem, the cranial nerve pathways in the peripheral nervous system, and the extraocular muscles in the orbit, with disease at any of these sites manifesting clinically as an eye movement disorder. Normal eye movements are directly controlled by the ocular motor cranial nerves (CN III, IV, and VI) in coordination with indirect input or sensory stimuli derived from other cranial nerves. However, the radiologist should be aware that the imaging findings in many of these conditions when taken in isolation from the clinical history and symptoms are often nonspecific. Imaging plays an important role in excluding, in some cases, and detecting, in others, a specific cause responsible for the clinical presentation. However, detecting the presence of ocular dysmotility may not be sufficient to pinpoint the exact cause of eye restriction. The presence of restricted eye movement can be detected clinically with quick, easily performed, noninvasive maneuvers that assess medial, lateral, upward, and downward gaze. Extraocular eye movement disorders are relatively common and may be a significant source of discomfort and morbidity for patients.
0 Comments
Read More
Leave a Reply. |
 RSS Feed
RSS Feed
